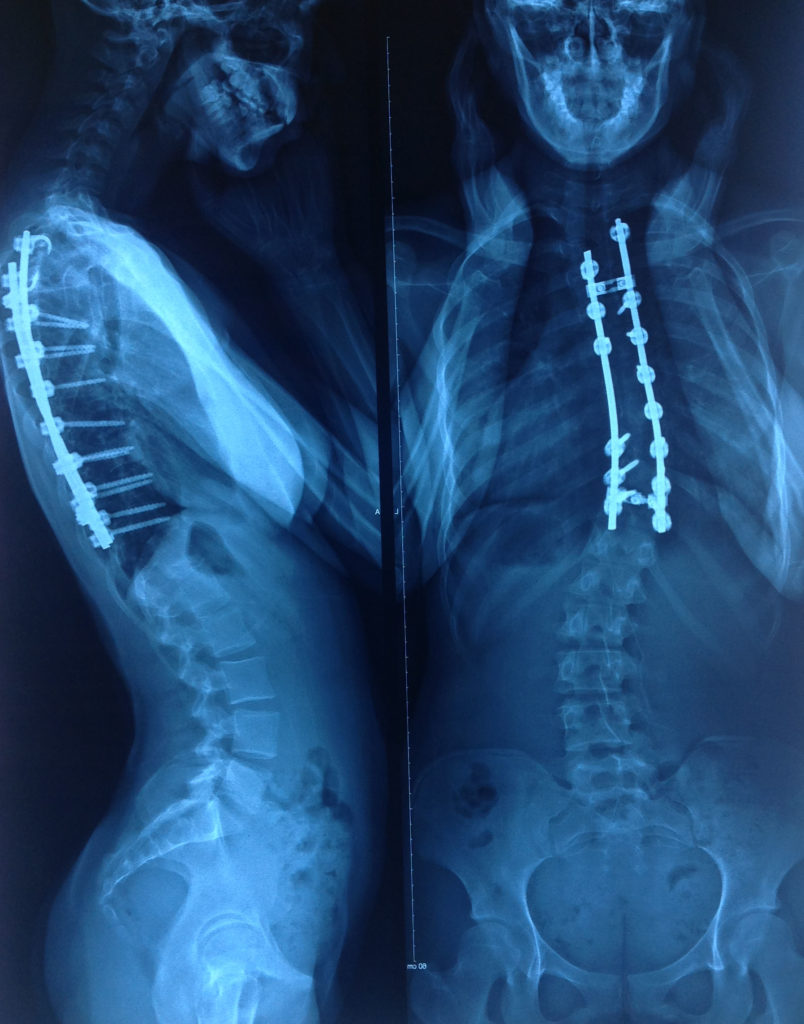
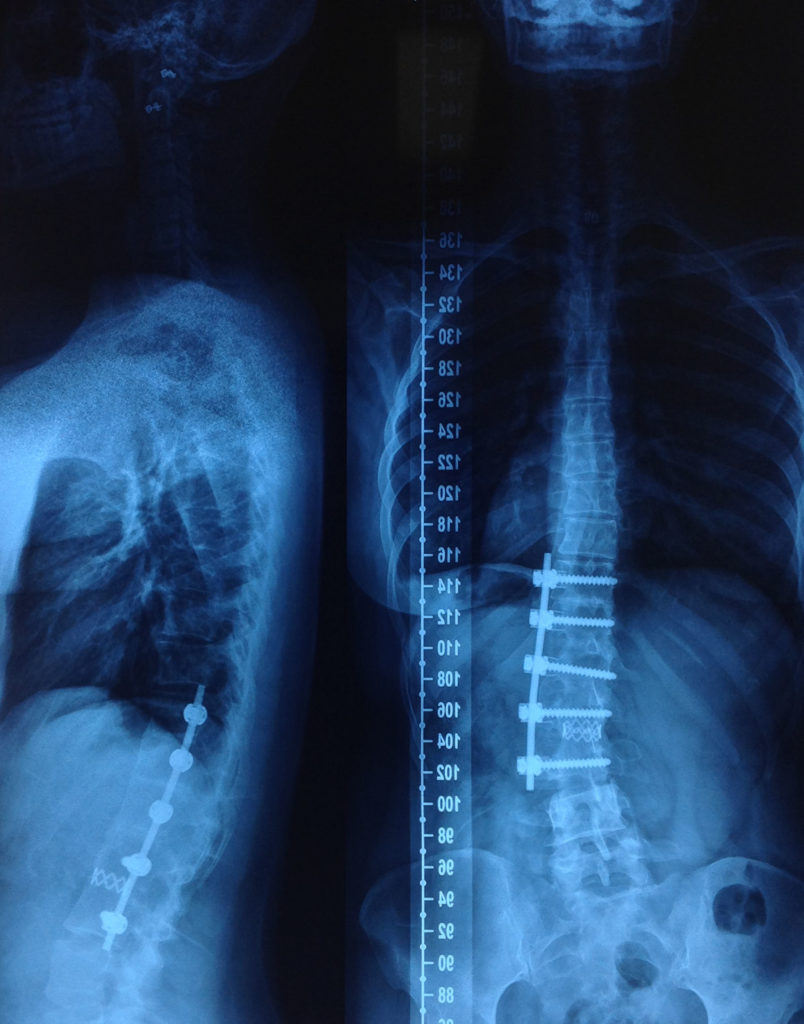
There are different types of surgery for scoliosis
Surgery for scoliosis is often recommended when curves exceed 50 degrees Cobb or there is deteriorating neurologic symptoms, significant lung function impairment or substantial restriction in the activities of daily living.
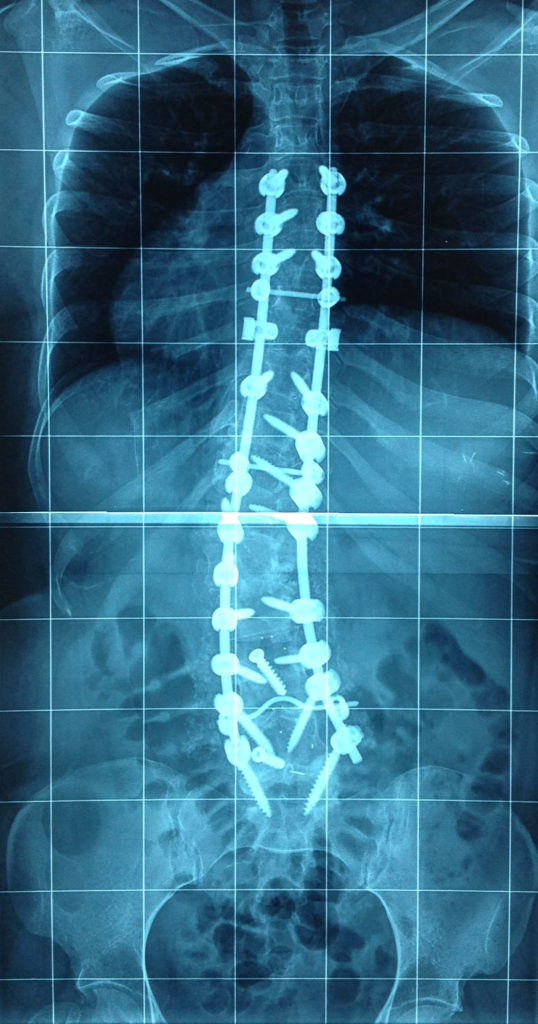
We work with many children and adults whom have had surgery. The most common type of surgery for scoliosis currently is posterior spinal fusion, where the surgeon accesses the spinal column via the back and attach the instrumentation to the posterior vertebral structures. They use screws and rods to bring the spine to as corrected an alignments as possible.
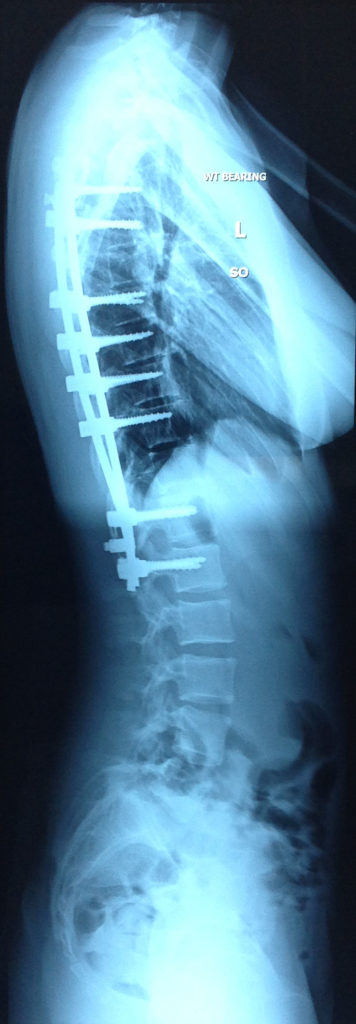
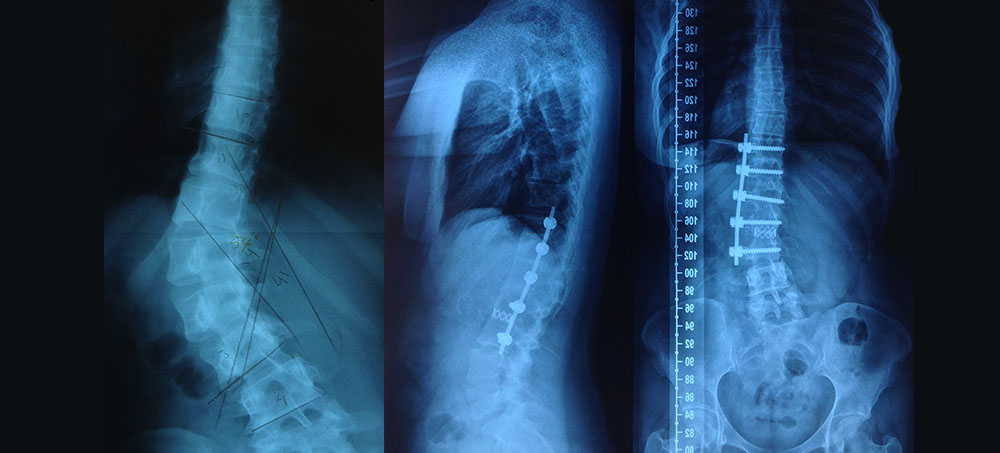
Another type of scoliosis surgery is anterior spinal fusion (pictured above). The surgeon enters the body from the lateral ribcage and attaches the instrumentation to the anterior part of the vertebrae, the vertebral body. Bone grafts are usually either taken from a section of the patient’s pelvis, ribs or from a bone bank.
Often pre-surgery x-rays are taken of the patient in side bending or whilst under traction to give the surgeon an indication of how corrected they may be able to get the spine with the fusion.
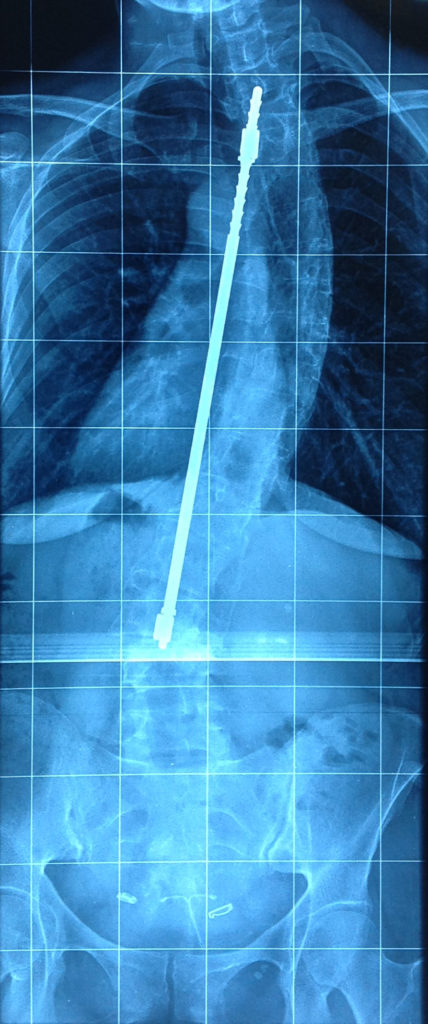
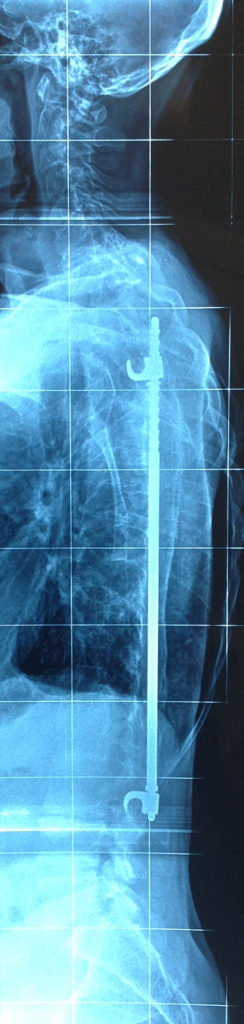
A popular past surgery type that is not routinely performed any more is the Harrington Rod surgery. This was ceased in mainstream surgery due to a crankshaft phenomenon where, despite the surgery, some curves continued to progress, especially the rotational component. This is believed to have occurred due to the anterior aspect of the spine continuing to grow after the posterior aspects were fused.
Applications/aims of PSSE after scoliosis surgery:
-
- Reduce degeneration of the adjacent unfused spinal segments
Early degeneration of the unfused spinal segments either side of the fusion is a well-known occurrence that through good spinal condition and movement habits is hoped to be reduced. This is achieved by providing muscle support in the deep spinal stabilization muscles as well as those muscle systems responsible for maintaining adequate elongation and minimizing compressive loads. Training correct biomechanics and movement habits is paramount to minimize unnecessary stress on the unfused spinal regions.
(pics of adjacent joint degeneration)
-
- Assist alignment of the unfused secondary curves
Often just the primary or structural curves are fused surgically and the secondary or compensatory curves are left unfused in the hope that they will reduce gradually themselves as some do. In some instances they do not however and improving the alignment of these curves and the associated aesthetics is a goal of the scoliosis specific exercises.
-
- Assist rib cage shape
When a curve has been present for a length of time, the muscles and associated soft tissues in the regions of collapse (the concavities) often become shortened. We see this often in the intercostal muscles between the ribs, where their ongoing tightness causes the ribs to remain very close, despite the spine itself being straightened by the fusion and the concavity being removed/reduced. This restriction in rib mobility can cause areas of the rib cage to remain sunken aesthetically, may cause pain issues and effect lung function. The Schroth-based method targets rib cage mobility very specifically with its unique breathing techniques for which it is well known.
-
- Aid lung function recovery (reduced by 50% for 2 years following surgery)
Reduction in lung function after scoliosis spinal surgery is well documented. Part-taking in appropriate cardio work, at the approved timeframes as specified by your surgeon will help to restore lung function. Should recurrent chest infections or pneumonia occur, specific rib expansion exercises, as utilised in BSPTS Schroth-based exercises, directed to the regions of restriction may be helpful.
treatments
Scoliosis Conditions Treated
Other Conditions Treated